The 3 Types of Thyroidectomy Explained
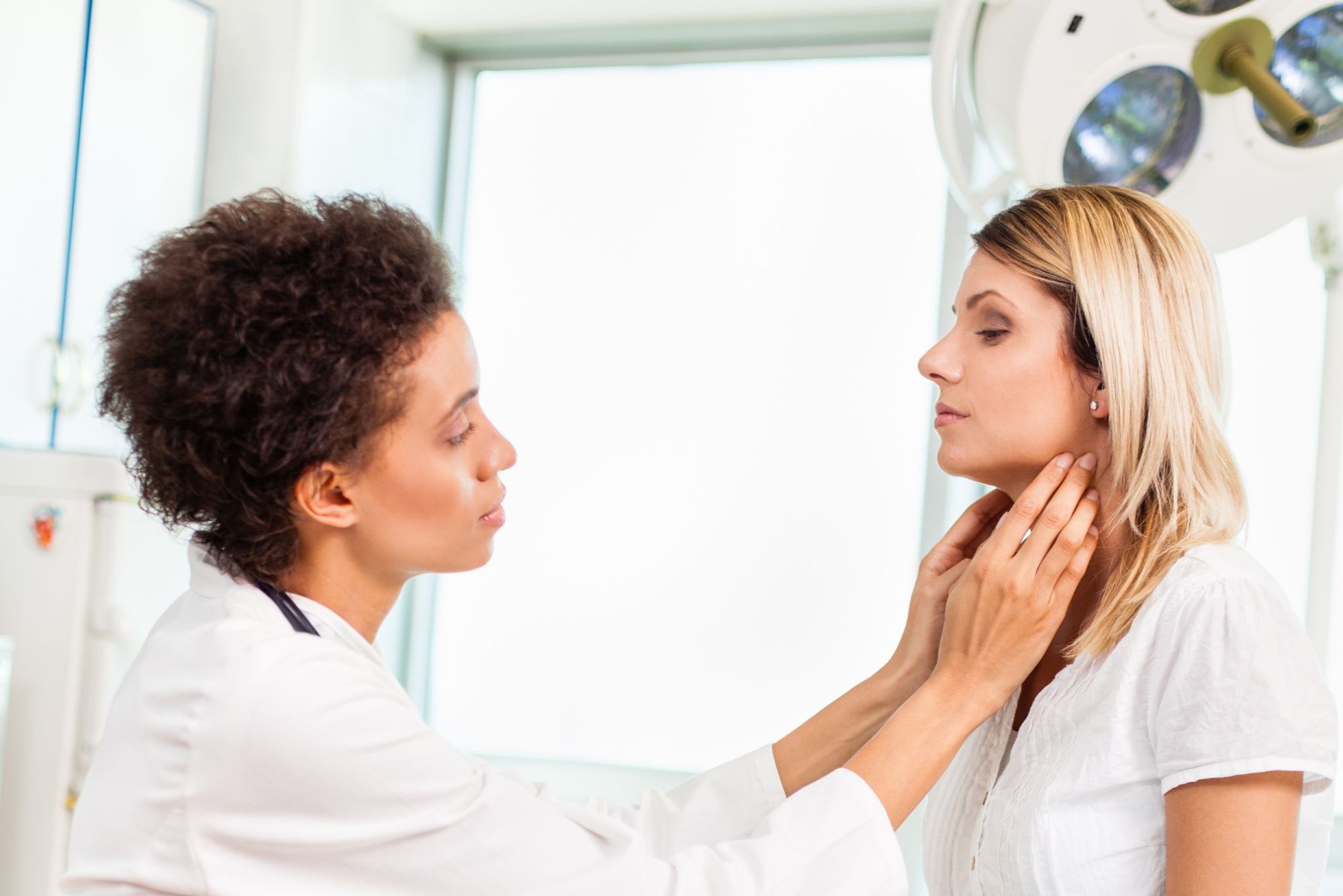
A thyroidectomy seems like a simple enough procedure, right? “Thyroid” refers to the butterfly-shaped gland that sits at the base of your neck, and “-ectomy” means “to remove.”
But wait. Once you start to research this procedure, you find out there are different types of thyroidectomy: subtotal thyroidectomy, partial thyroidectomy, hemithyroidectomy, total thyroidectomy. What do all these terms mean?
In reality, there are only three types of thyroidectomy, and really only two that we commonly perform today. So let’s take a look at the three types of thyroidectomy, the differences between them, and when a thyroidectomy is needed.
Who Needs a Thyroidectomy?
The thyroid is a small organ with a lot of power. It affects many metabolic functions in your body — like breathing and body temperature — and it releases vital hormones to keep your body running.
Sometimes, however, the thyroid can develop problems. In these cases, one of the types of thyroidectomy can become necessary.
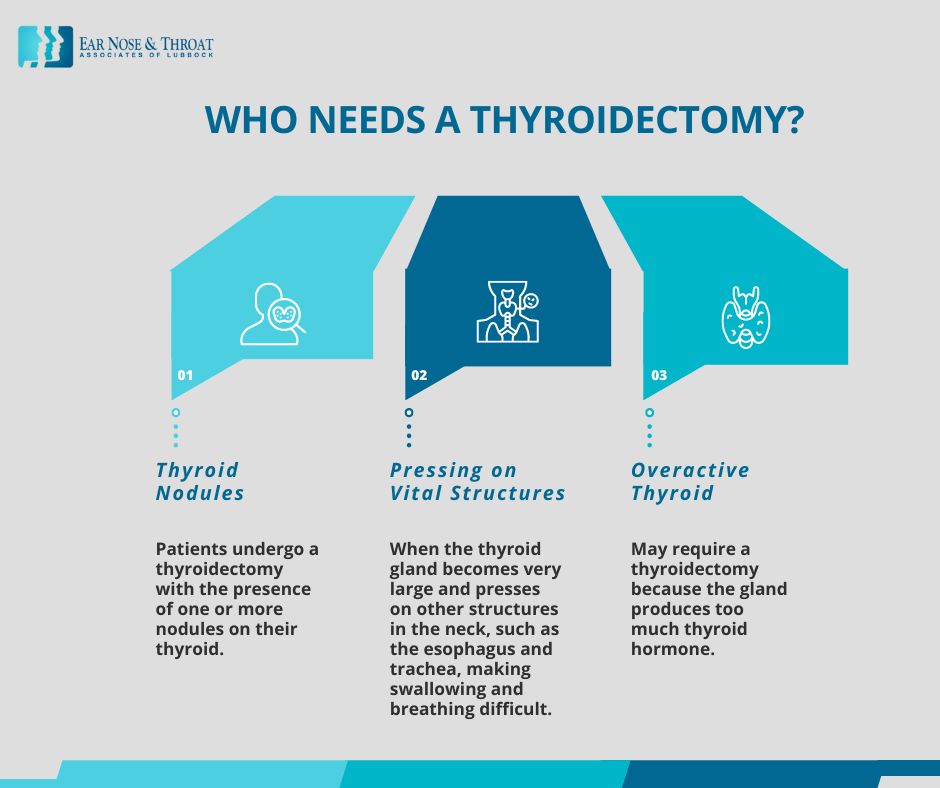
Problem 1: Thyroid Nodules
The most common reason patients undergo a thyroidectomy is the presence of one or more thyroid nodules. Thyroid nodules are extremely common, and their incidence increases with age. In fact, ENT doctors often use age as a reference point for how common nodules are. For example, about 50% of 50-year-olds have nodules on their thyroid.
When your doctor notices a suspicious nodule on your thyroid gland, they may want to perform further testing, such as an ultrasound and/or a fine-needle aspirate (a type of biopsy).
A system called TI-RADS classifies thyroid nodules according to how concerning they are on a scale of one through six. A TI-RADS score of three or more usually indicates the need for a needle biopsy, after which a pathologist looks at the nodule cells under a microscope to determine whether they are cancerous. If the pathologist’s findings are inconclusive, then genetic testing can be performed as well.
More than 90% of nodules in adults will not be cancerous, but it’s crucial to identify the ones that are.
Problem 2: Enlarged and Pressing on Vital Structures
Another reason for a thyroidectomy is when the thyroid gland becomes very large and presses on other structures in the neck, such as the esophagus and trachea, making swallowing and breathing difficult.
Problem 3: Overactive Thyroid
People with certain thyroid diseases may require a thyroidectomy because their gland produces too much thyroid hormone. This is often impossible to control medically, making removal of the thyroid gland the best option. Graves’ disease is one example of such a condition.
Subtotal Thyroidectomy / Partial Thyroidectomy
In past years, subtotal thyroidectomies (also called partial thyroidectomies) were common for patients with overactive thyroid glands from conditions like Graves’ disease. The thought for this surgery was that if the entire gland wasn’t removed, the patient wouldn’t need to rely on prescription thyroid medication for the rest of their life.
However, the thinking surrounding this issue has changed in more recent years. Thyroid hormone replacement therapy is now quite safe, effective, and affordable, and it’s difficult to accurately estimate how much of the thyroid gland to remove and how much to leave.
As a result, the subtotal thyroidectomy or partial thyroidectomy is almost obsolete in our practice. While this procedure was an effort to minimize possible thyroidectomy complications, we now have better ways to minimize this risk, such as choosing a high-volume thyroid surgeon and closely following their postoperative instructions.
The other two types of thyroid surgeries listed below are much safer.
Hemithyroidectomy / Total Thyroid Lobectomy
A hemithyroidectomy, also called a total thyroid lobectomy, removes only one side of the thyroid gland, leaving the other lobe intact.
A hemithyroidectomy is usually performed when a patient has a suspicious-looking thyroid nodule. Sometimes, despite an ultrasound and a fine needle aspiration, it’s still hard to determine whether a nodule is cancerous. In many cases, once we remove the side of the thyroid with the nodule, we can immediately analyze it to find out whether cancer is present.
If no cancer is discovered, then the surgery is finished and the patient continues on with one thyroid lobe remaining. Often, they may not even need to take supplemental thyroid hormone because the existing side compensates for the side that was removed.
If cancer is discovered in the operating room like this, the surgeon may need to continue on to a total thyroidectomy. If you’re going in for a hemithyroidectomy, your thyroid surgeon will discuss the possibility of a total thyroidectomy with you before your surgery.
In the case of thyroid cancer, removing the entire thyroid allows for treatment with radioactive iodine, which can destroy any remaining microscopic disease.
Total Thyroidectomy
A total thyroidectomy is exactly what it sounds like: the removal of both sides (lobes) of the thyroid gland.
As mentioned above, a total thyroidectomy is often needed when cancer is found on one side of the thyroid. Another indication for a total thyroidectomy is when the thyroid gland grows to be extremely large and compresses the esophagus and trachea. In this case, removal relieves pressure in the neck, aids in swallowing and breathing, and serves a cosmetic function as well.
A total thyroidectomy is also the new standard type of thyroidectomy for controlling overactive thyroid glands due to conditions like Graves’ disease.
Looking for More Information About the Different Types of Thyroidectomy?
If you’ve been told that you may need a thyroidectomy, you may be a little anxious about the procedure and want as much information as possible.
We’ve written several articles to provide you with useful information about thyroid surgeries. Take a look at our guide to choosing a thyroid surgeon and our ultimate guide to thyroidectomies. We also have a post about how to manage and avoid thyroidectomy complications, tips to speed your thyroidectomy recovery process, and what you need to know about the scar you’ll have after thyroid surgery.
Dr. Scolaro is a board-certified Otolaryngologist servicing the South Plains area. He has been practicing in Lubbock since 1990 and has earned a reputation as a skilled and experienced surgeon. He currently serves as the Medical Director for Covenant High Plains Surgery Center campuses, is a member of Covenant Health Partners and is an adjunct faculty professor for Texas Tech University Health Sciences Center School of Medicine. Learn more about Dr. Scolaro.
Categories: